Ultrasound, also called ultrasound scanning or sonography, is an imaging method that uses sound waves to create an image of a part of the body. A computer program is used to analyze the echoes of sound waves sent into the body and generates an image on screen. 1
Unlike mammograms, which use radiation (x-rays), ultrasounds expose the body region of interest to high-frequency sound waves. Ultrasound images are captured in real time; that is, not only do they show the structure of a particular part of the body, but they can also show movement of the body's internal organs as well as blood flowing through vessels.2
View a documentary on breast ultrasound.
Below is a list of the information included on this page:
- How it Works
- What to Expect
- Test Results
- Doppler Ultrasound
- Ultrasound for Breast Cancer
- Ultrasound for Uterine and Ovarian Cancer
- Benefits and Disadvantages
- Frequently Asked Questions (FAQ)
How It Works
Amplitude: strength of the signalWhat instruments are used?
Ultrasound scanners consist of a stand with a computer and electronics, a display screen to show the image, and a hand-held transducer that is used to scan the body. The transducer emits high-frequency sound waves and receives the returning waves (echoes). The computer collects the echoes and creates an image on the screen.2 In creating the final image, the computer analyzes several characteristics of the returned sound waves:
- Frequency: the number of waves received per second
- Time Delay: the time it takes for the signal to return from the targeted region to the transducer
How does ultrasound work?
Ultrasound imaging is based on the same principles of physics that bats use to locate their prey. When the transducer emits a sound wave and it hits an object, the wave bounces off the object. By measuring the echo waves, the computer can determine how far away the object is, its size, shape, uniformity, and consistency (whether the object is solid, fluid-filled, or a mixture).2
Ultrasound uses sound waves. The waves bounce off of different kinds of tissues differently. They can be used to identify possible cancer and guide treatments.
What To Expect
For most ultrasound exams, the patient lies face-up on the examination table. A clear gel is applied to the area being examined. The gel allows the transducer to have ideal contact with the body by eliminating all air pockets. The physician will then firmly press the transducer against the skin and slowly move it around the area of interest. After the ultrasound scanning is complete, the gel will be wiped off the patient's skin and the patient can leave. 2
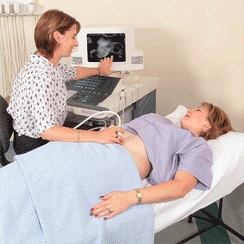
Image courtesy of Brent Burbridge, MD Saskatoon Medical Imaging, Saskatoon Canada.
In some ultrasound exams, physicians insert the transducer inside the body to obtain useful results. In these cases, the transducer is attached to a probe and then placed into one of the body's openings. For example, a transesophageal echocardiogram is taken by placing the transducer into the esophagus to get an image of the heart. A transrectal ultrasound involves placing the transducer into a man's rectum to obtain images of the prostate. In a transvaginal ultrasound, the transducer is inserted into a woman's vagina to view the uterus and ovaries. 2
Preparation
If you are getting an ultrasound, wear loose-fitting, comfortable clothes. All clothing and jewelry covering the area being examined will have to be removed. In some cases, you may be asked to wear a gown for the procedure. 2
Results
Besides allowing visualization of a lesion, an ultrasound is also the only non-invasive way to determine if a suspicious lump is a benign, fluid-filled cyst, or whether it is a solid cancerous mass. A cyst cannot be correctly diagnosed with only a physical exam or mammography. Ultrasounds are also helpful because they can be used to help guide a needle during a biopsy. 3 Research with women who have either breasts that are too dense for mammograms, or are at an increased risk for breast cancer, has shown that ultrasounds can also distinguish between benign and malignant masses. 4, 5
Ultrasounds are good exams to gain important information about a suspicious mass. However, they are not used for primary screening because of several factors. Because a well trained professional must administer the exam and interpret the results, they are expensive and the interpretation can vary on the evaluator. There is also a higher incidence of incorrectly identifying a mass as cancerous, a false positive, than with mammography. 6, 7 Additionally, ultrasounds are unable to detect microcalcifications (small mineral deposits in the breast that indicate the possibility of malignancy). 4 All cancers do not show up on ultrasounds, and in some cases, an ultrasound will not provide enough information for a physician to decide whether or not a mass is malignant, and a biopsy will be recommended.
The images below show examples of ultrasound results.
Left- liver containing metastatic cancer growths; Right- an ovary containing a large irregularly shaped mass.
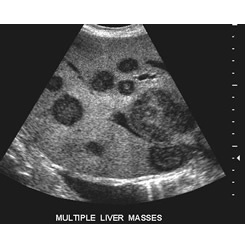
Image courtesy of Brent Burbridge, MD Saskatoon Medical Imaging, Saskatoon Canada
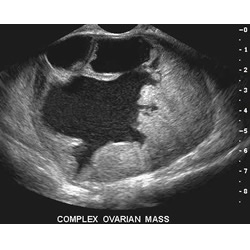
Image courtesy of Brent Burbridge, MD Saskatoon Medical Imaging, Saskatoon Canada
In the detection of breast cancer, ultrasound imaging is an extremely useful tool, but is not a substitute for mammography.8, 9Learn more about breast ultrasound.
Doppler
A Doppler ultrasound which is often included as a part of an ultrasound breast exam, allows visualization of blood flow (or lack of blood flow) in a breast mass. It allows the physician to assess the blood supply in a breast lesion.8 There are three types of Doppler ultrasounds:
- Color Doppler- the computer uses measurements from the ultrasound machine to produce an image with many colors so that the speed and direction of blood flow can be seen.
- Power Doppler- this is a recently developed technique that is more sensitive than the color Doppler. The power Doppler can provide more information and detail about blood flow, and is exceptionally good for visualization of vessels located inside organs.
- Spectral Doppler- this imaging technique provides a graphic display of blood flow in terms of distance traveled per unit of time.
Doppler ultrasounds are important in the diagnosis of breast lesions because a malignant (cancerous) mass is likely to have blood flow irregularities.2, 10
Shown below is a normal Doppler ultrasound of a liver
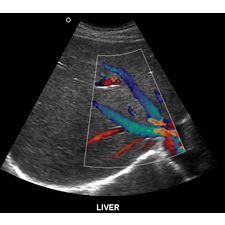
Image courtesy of Brent Burbridge MD, Saskatoon Medical Imaging, Saskatoon Canada
For Specific Cancers: Breast
Breast ultrasounds are used mainly to further examine breast abnormalities detected by a physician during a physical exam or mammogram. 8, 11
The single most important factor affecting the accuracy of ultrasounds is breast density. In a study of 3,626 women with dense breasts, ultrasounds were used instead of physical exams to detect abnormalities. This study found that the number of breast cancer cases found by ultrasound was 17% higher than those found by physical exams. 12
The images below show ultrasound results for a normal breast (left) and a breast containing a cyst (right)
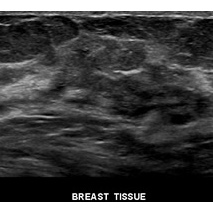
Image courtesy of Brent Burbridge, MD Saskatoon Medical Imaging, Saskatoon Canada.
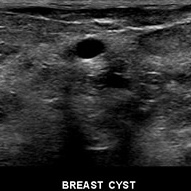
Image courtesy of Brent Burbridge, MD Saskatoon Medical Imaging, Saskatoon Canada.
Over 50% of women under the age of 50, and about 33% of women over 50 have dense breasts.8 Young women have breasts that are dense and full of milk glands, sometimes making mammograms difficult to interpret. For this reason, many physicians will recommend that women under the age of 30 who have a lump in their breast get an ultrasound exam before a mammogram.13
Ultrasound is also used today for women with breast implants. Since there is very little tissue around a silicone implant to be x-rayed, mammograms are not always useful to detect abnormalities. Ultrasounds are also used as an alternative imaging method for pregnant women because they should not be exposed to x-rays.8
For Specific Cancers: Uterine And Ovarian
Transvaginal (endovaginal) ultrasound screening provides high-resolution images of the uterus and ovaries. This allows the entire uterus to be observed for cancer of the endometrium. Ovarian cancer can be detected before the lesions are palpable. The procedure involves the insertion of a small probe into the vagina. The probe then sends out ultrasound waves that are used to generate an image of the tissues.14 Signs of possible cancer that can be detected this way include: masses and altered (low-velocity) blood flow.15
Three-dimensional (as opposed to two-dimensional) Doppler imaging has been shown in trials to significantly improve the specificity of the screening. This technique allowed benign masses to be distinguished from malignant ones with more accuracy.15
Currently, transvaginal ultrasound screening does not have high enough specificity and sensitivity to significantly decrease mortality in the general population. The costs are high and ovarian cancer is not very prevalent. However, the screening is recommended for women at high risk of developing ovarian cancer, such as those with a family history of breast and ovarian cancer and/or those who carry a BRCA-1 or -2 mutation.16
Benefits And Disadvantages
Benefits of ultrasound:
- Can detect lesions in women with dense breasts when mammograms cannot.8
- Can help identify the nature of a lesion that is unclear from a mammogram.8
- Widely available, and less expensive than a mammogram.17
- The only way to tell the difference between a cyst and a solid mass without using a needle to draw out fluid (non-invasive).17
- Patient is never exposed to radiation during an ultrasound, allowing pregnant women to use this imaging technique.3
- Can use ultrasound to detect blood flow through vessels.2
- Most ultrasound exams are quick and painless.2
- Ultrasounds do not cause any health problems, and there are no known harmful effects to humans.2
Disadvantages of ultrasound:
- Ultrasound results may identify a potential area of concern that is not malignant. These false-positive results could lead to more procedures, including biopsies, that are not necessary 8. Preliminary data from a trial being conducted showed that there was a higher rate of false-positive results with ultrasounds than with mammography (2.4%-12.9% for ultrasound and 0.7%-6% for mammography).4
- Although ultrasound is often used in an attempt to prevent an invasive measure for diagnosis, sometimes it is unable to determine whether or not a mass is malignant, and a biopsy will be recommended.8
- Many cancers cannot be detected via an ultrasound.8
- Calcifications that are visible on mammograms are typically not visible on ultrasound scans. This may prevent early diagnosis of a portion of breast cancers that begin with calcifications.18
- Ultrasounds are not available everywhere, and not all insurance plans cover them.8
- An ultrasound requires a highly experienced and skilled operator to detect a malignant lump, as well as good equipment. If the cancerous tissue is not detected at the time of the scan, it will not be caught as early as possible. The ACR-accredited facilities database is a good way to determine the expertise of a facility in ultrasound imaging.4, 8
Frequently Asked Questions
- In women with dense breasts ultrasound provides an alternative view of the breast that is easier to interpret
- In pregnant women to protect the fetus from mammography radiation exposure
- In women with breast implants, the implants may distort the image produced by mammography
- In women at high risk for breast cancer because of family history
- 1 American Cancer Society. Accessed on October 3, 2010 [http://www.cancer.org]
- 2abcdefghij "Ultrasound- General." Radiology Info (07-10-2007) [http://www.radiologyinfo.org/en/info.cfm?pg=genus&bhcp=1]
- 3ab "Mammograms and Other Breast Imaging Procedures." American Cancer Society (08-03-2010) [http://www.cancer.org/Healthy/FindCancerEarly/ExamandTestDescriptions/MammogramsandOtherBreastImagingProcedures/index?sitearea=PED]
- 4abcd Elmore JG et al. "Screening for Breast Cancer." JAMA (2005). 293: 1245-1256. [PUBMED]
- 5 Gordon PB. et al. "Malignant breast masses detected only by ultrasound. A retrospective review." Cancer (1995) Aug 15;76(4):626-30. [PUBMED]
- 6 Gordon PB. Ultrasound for breast cancer screening and staging. Radiol Clin N Am. 2002;40:431-441 [PUBMED]
- 7 Irwig L, Houssami N, van Vliet C. New technologies in screening for breast cancer: a systematic review of their accuracy. Br J Cancer. 2004;90:2118-2122 [PUBMED]
- 8abcdefghijkl "Breast Ultrasound" Radiology Info (07-10-2007) [http://www.radiologyinfo.org/en/info.cfm?PG=breastus]
- 9 Sickles, EA. et al. "Benign breast lesions: ultrasound detection and diagnosis." Radiology (1984) May;151(2):467-70. [PUBMED]
- 10 Peters-Engl C. et al. "The use of colour-coded and spectral Doppler ultrasound in the differentiation of benign and malignant breast lesions." Br J Cancer. (1995) Jan;71(1):137-9. [PUBMED]
- 11 Kolb TM, et al. "Comparison of the Performance of Screening Mammography, Physical Examination, and Breast US and Evaluation of Factors that Influence Them: An Analysis of 27,825 Patient Evaluations." Radiology (2002) 225(1):165-175. [PUBMED]
- 12 Kolb TM, et al. "Occult cancer in women with dense breasts: detection with screening US-- diagnostic yield and tumor characteristics." Radiology (1998). Apr; 207(1): 191-9. [PUBMED]
- 13 https://acsearch.acr.org/docs/69495/Narrative/
- 14 Van Nagell JR, Higgins RV, Donaldson ES, et al. "Transvaginal Sonography as a Screening Method for Ovarian Cancer." Cancer (1990). 65: 573-577. [PUBMED]
- 15ab Cohen LS, Escobar PF, Scharm C, Glimco B, Fishman DA. "Three- Dimensional Power Doppler Ultrasound Improves the Diagnostic Accuracy for Ovaian Cancer Prediction." Gynelogical Oncology (2001). 82:40-48. [PUBMED]
- 16 Hensley ML, Castiel M, Robson ME. "Screening for Ovarian Cancer: What We Know, What We Need to Know." Oncology (Huntington) (2000). 11:1601-1607. [PUBMED]
- 17ab "If Breast Cancer is Suspected. American Cancer Society (8-03-2010). [http://www.cancer.org/Treatment/UnderstandingYourDiagnosis/ExamsandTestDescriptions/ForWomenFacingaBreastBiopsy/breast-biopsy-mammograms]
- 18 Bitencourt, A., Graziano, L., Guatelli, C., Albuquerque, M., & Marques, E. (2018). Ultrasound-guided biopsy of breast calcifications using a new image processing technique: initial experience. Radiologia Brasileira, 51(2), 106–108. http://doi.org/10.1590/0100-3984.2017.0054 (Original work published December 2018) [PUBMED]


