
Magnetic Resonance Imaging (MRI) is a non-invasive way to view organs, tissues, bones, and other structures inside the body. It uses strong magnetic fields and radio waves to produce internal images of the body. Unlike X-ray and CT scans, MRI machines produce cross sectional, 3D images of the body without using the use of radiation. Doctors often use MRI to view parts of the body that are hard to see with other imaging techniques such as x-rays, ultrasound, or computed tomography (CT) scans. MR imaging is used to diagnose many different types of diseases including heart and vascular disease, stroke, muscle and skeletal (bone) disorders and cancer.1, 2
Below is a list of the information included in this page:
- MRI Instruments
- Preparation & Precautions for MRI
- What to Expect During an MRI
- The MRI Exam Process
- MRI Results
- Benefits and Disadvantages of MRI
- Cancer Specific MRI: Breast
MRI Instruments
An MRI machine is a large, cylinder shaped machine that contains a very strong donut-shaped magnet. Magnets are commonly measured using gauss and an MRI magnet can be up to 20,000 gauss (common refrigerator magnets are around 10 gauss). However, even a magnet of 20,000 gauss is not harmful to humans (much stronger magnets have been tested with no ill effects). The patient lies on a bed that moves in and out of the machine during the process. The machine is connected to a computer that receives signals from the MRI unit. The computer interprets the signals and generates a 3-D image of the patient's body.1, 2
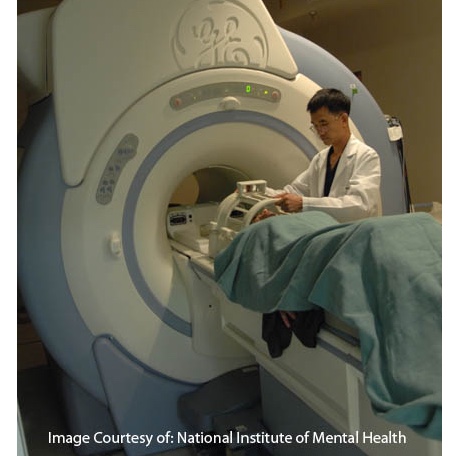
MRI, unlike x-rays and CT scans, does not use ionizing radiation. Instead, it uses radio waves that interact with specific molecules in the body (protons, the nuclei of hydrogen atoms).3 During the exam, radio signals are repeatedly turned on and off. The energy in the radio waves is absorbed by different atoms in the target area and reflected back out of the body. When the radio waves are reflected off tissues in the patient's body, they generate signals that are detected by the MRI machine. These signals are sent to the MRI computer, which collects the signals from the coil and combines them to create a 3-D image.4
Preparation & Precautions for MRI
The MRI unit is an extremely strong magnet, so patients should avoid wearing jewelry and other accessories because they could interfere with the machine's magnetic field. The following items are not allowed to enter the exam room:
- Jewelry, watches, credit cards, and hearing aids (all can be damaged)
- Pins, hairpins, metal zippers, and similar metallic items (can alter images taken)
- Removable dental work
- Pens, pocketknives, eyeglasses1
Most of the time, MRI is safe for patients who have implants made of metal. However, the technologist should know if the patient has medical/electronic devices in his/her body including:
- artificial heart valves
- implanted drug infusion ports
- implanted electronic devices
- artificial limbs or metallic joint prostheses
- implanted nerve stimulators
- metal screws, plates, or surgical staples3
If there is any doubt about the presence of metal in the patient's body, an x-ray should be taken.
Very rarely, dyes used in tattoos contain iron which may heat up during an MRI, so the patient should communicate any concerns with his/her physician.
Other things to keep in mind before you receive an MRI:
- Patients with claustrophobia or anxiety may want to request a mild sedative from their physicians.3
- If an MRI scan will involve contrasting agent, the patient should tell the physician about any allergies including hay fever, hives, allergic asthma, or food and drug allergies.5
- The radiologist should also be informed if the patient has any type of serious health problems such as kidney disease or sickle cell anemia because it may affect whether or not contrasting agent is used with the MRI scan.
- Women who may be pregnant may be asked to give a urine sample beforehand since risks of MRI scanning to the fetus are not yet known. Pregnant women should not have an MRI exam unless the potential benefit from MRI is greater than the potential risks to the fetus.1
- Continue taking normal medications prior to the exam unless told otherwise by the physician.
Those who have a cardiac pacemaker, defibrillator, or ear implant absolutely cannot be scanned and should take caution to not enter the MRI exam room because the strength of the magnet could cause serious problems.1
What to Expect During an MRI
During an MRI exam, the patient is placed on a table that rolls into the MRI unit. During the exam, the radiologist and technologist will leave the MRI room and observe from an adjoining room.1
An exam usually consists of two to six imaging "sequences", with each sequence lasting less than fifteen minutes. Depending on the type of image needed, patients undergo a number of scans to obtain images from different angles and viewpoints. One session of magnetic resonance imaging can produce hundreds of images of the body; side to side, top to bottom, and front to back.4 When the images are combined by the computer, a detailed picture is created that allows the radiologist to see areas inside the body.
In some cases, a physician may decide to use a contrast agent known as gadolinium DTPA to help enhance the image quality of the MRI scan. This non-radioactive contrast agent improves the strength and clarity of the images by emphasizing the tumor-like qualities of any suspicious masses.5, 2 Ask your doctor about side effects of the gadolinium-based contrast material if you have kidney problems.
If a contrasting agent is used, an intravenous (IV) line will be inserted into the patient's hand or arm, which will allow the radiologist to inject the contrasting substance directly into the patient's body at the appropriate time. The contrasting agent often creates a cooling sensation at the site of injection and throughout the body. The patient may also experience some discomfort at the injection site.1
The MRI Exam Process
During an MRI scan the patient will hear loud noises that are generated within the MRI unit while images are being produced. The patient can usually ask for earplugs to reduce the sound of the MRI scanner. Some of the newer scanners have music to help the patient pass the time. They also may be air-conditioned and have lights inside.3
Although most patients will spend between 30 and 60 minutes in the MRI machine, they are allowed to take breaks between sequences so that they are not required to lie still for the entire time.1 Throughout the exam the patient will be able to talk to both the radiologist and the technologist, though they will both leave to observe from an adjacent room during the actual imaging process. Additionally, some facilities allow for a relative or close friend to stay near the patient during an exam.
MRI is normally a pain-free process that requires no recovery period afterwards. Occasionally patients have side effects from the contrast material such as nausea and local pain, and, very rarely, patients can have an allergic reaction to the agent that results in hives and itchy eyes. Nursing mothers should avoid breastfeeding for 36-48 hours after having an MRI scan using contrasting agent.5 Those with kidney problems should avoid gadolinium-based contrast material. Most people who have an MRI scan are able to resume their normal activities and diet immediately after the exam.1
MRI Results
Magnetic resonance imaging helps identify tumors by magnifying the differences in water content and blood flow between tissues. Malignant tumors grow their own network of blood vessels via angiogenesis; this gives them a larger blood supply than the surrounding tissue. Contrast material highlights this concentration of blood vessels to help pinpoint malignant growths.1
When contrast agent is not used an MRI can show:
- The shape, size, appearance, and location of organs, bones, and joints
- The presence of abnormal growths
- Signs of inflammation or infection3
When contrast agent is used MRI can show:
- size and location of benign or malignant growths
- enlarged lymph nodes
- changes in blood flow
- extracellular volume 1, 5
As useful as MRI is, it cannot always accurately differentiate between cancerous and non-cancerous lesions. As an example, MRI cannot detect microcalcifications, which may be indicators of the primary stages of breast cancer.4 Therefore, it is very important that patients consult their physicians about which screening method is best suited for them.
Benefits and Disadvantages of MRI
Benefits of MRI:
- MRI is non-invasive and does not use radiation
- MRI does not involve radiation
- MRI contrasting agent is less likely to produce an allergic reaction that may occur when iodine-based substances are used for x-rays and CT scans
- MRI gives extremely clear, detailed images of soft-tissue structures that other imaging techniques cannot achieve
- MRI can easily create hundreds of images from almost any direction and in any orientation
- Unlike techniques that examine small parts of the body (i.e. ultrasound or mammography) MRI exams can cover large portions of the body
- MRI can determine if a cancer has spread, and help determine the best treatment
Disadvantages of MRI:
- MRI is expensive ($1000-$1500)
- MRI will not be able to find all cancers (i.e. breast cancers indicated by microcalcifications)
- MRI cannot always distinguish between malignant tumors or benign disease (such as breast fibroadenomas), which could lead to a false positive results
- MRI is not painful, but the patient must remain still in an enclosed machine, which may be a problem for claustrophobic patients
- An undetected metal implant in a patient’s body may be affected by the strong magnet of the MRI unit
- There is a small chance that a patient could develop an allergic reaction to the contrasting agent, or that a skin infection could develop at the site of injection
- If a patient chooses to be sedated for the scanning, there is a slight risk associated with using the sedation medication
Cancer Specific MRI: Breast
Research is being conducted to investigate the benefits of MRI as a screening tool for breast cancer detection (as a companion to mammography, ultrasound, and other techniques). Although MRI is not recommended as a substitute for mammography, a study done in 2004 found that in women with an inherited susceptibility to cancer (history of breast cancer in the family), MRI was more sensitive than mammography in detecting tumors.6
Another earlier study from 2001 found that breast MRI was capable of detecting early breast cancer with 94%-100% sensitivity. Additionally, out of 196 women who were at high risk for hereditary breast cancer, MRI was able to identify six stage I invasive cancers and one non-invasive cancer, but ultrasound only detected three invasive cancers, mammography found two, and physical examination identified two. This study provided evidence that mammography may be less sensitive that MRI in detecting breast cancer for women carrying BRCA1 and BRCA2 mutations.7
Hartman et al. performed a study in 2004 in which they compared MRI and mammography in women at high genetic risk for breast carcinoma. They also found that breast MRI was able to detect high-grade ductal carcinoma in situ (DCIS) and high-risk lesions that mammography missed. Malignant lesions were found with MRI in three out of forty-one women while none were identified by mammography.8 These studies indicate that in some women, MR imaging is a better screening method than mammography. It is important to remember that the low specificity of MRI (which in most studies is between 50%-70%) is a major disadvantage because it results in unnecessary follow-up procedures.9
Over the last ten years, MRI technology has significantly improved yielding better image resolution and improved biopsy potential. Because physicians have gained more experience with breast MRI, they are now more skilled at interpreting the images.
Additionally, in the past, there have been cases in which physicians would suspect that their patients' distant metastases originated from a breast tumor. However, if the physicians were unable to detect the tumor with a physical exam or mammogram, the patients may have to have mastectomies. The availability of higher resolution images from MRI means that these primary tumors can be found more easily, and patients' breasts can be conserved.10
- 1abcdefghijk "MRI of the Body (Chest, Abdomen, Pelvis)." Radiology Info (accessed on 01-27-08) [http://www.radiologyinfo.org/en/info.cfm?pg=bodymr&bhcp=1]
- 2abc Barentsz J, Takahashi S, Oyen W, Mus R, De Mulder P, Reznek R, Oudkerk M, and Mali W. "Commonly used imaging techniques for diagnosis and staging." Journal of Clinical Oncology. 2006 Jul 10;24(20):3234-44. [PUBMED]
- 3abcde "Imaging (Radiology) Tests." American Cancer Society (accessed on 08-03-2010) [http://www.cancer.org/docroot/PED/content/PED_2_3X_Imaging_Radiology_Tests.asp?sitearea=PED]
- 4abc Margolis D., MD, Hoffman J., MD, Herfkens R., MD, Jeffrey R., MD, Quon A., MD, and Gambhir S., MD, PhD . "Molecular imaging techniques in body imaging." Radiology. 2007 Nov;245(2):333-56. [PUBMED]
- 5abcd Bellin, MF. "MR contrast agents, the old and the new." European Journal of Radiology. 2006 Dec;60(3):314-23. [PUBMED]
- 6 Kriege, M. et. al. "Efficacy of MRI and Mammography for Breast-Cancer Screening in Women with a Familial or Genetic Predisposition." N Engl J Med. 2004 Jul 29;351(5):427-37. [PUBMED]
- 7 Warner, E. et. al. "Comparison of Breast Magnetic Resonance Imaging, Mammography, and Ultrasound for Surveillance of Women at High Risk for Hereditary Breast Cancer." Journal of Clinical Oncology. 2001 Aug 1; 19(15): 3524-31. [PUBMED]
- 8 Hartman, AR. et al. "Breast magnetic resonance image screening and ductal lavage in women at high genetic risk for breast carcinoma." Cancer. 2004 Feb 1;100(3):479-89. [PUBMED]
- 9 Macura, K.J. "Patterns of Enhancement on Breast MR Images: Interpretation and Imaging Pitfalls." Radiographics. 2006 Nov-Dec;26(6):1719-34; quiz 1719. Review. [PUBMED]
- 10 Buchanan, C. L. et al. "Utility of Breast Magnetic Resonance Imaging in Patients with Occult Primary Breast Cancer." Ann Surg Oncol. 2005 Dec; 12(12): 1045-53. Epub 2005 Oct 25. [PUBMED]
