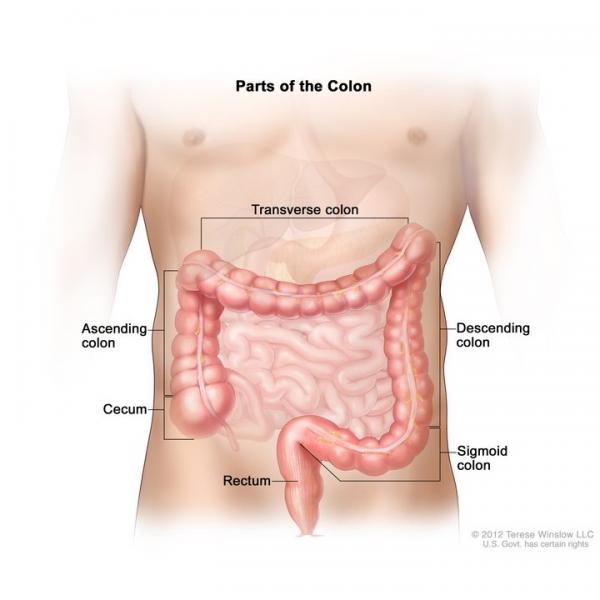
Colon cancer and rectal cancer, collectively known as colorectal cancer, have many similar characteristics and will be discussed as one cancer type in this section.
Colorectal cancer is currently the third most common cancer in both men and women. Incidence and mortality rates have been declining since the 1980's, partially due to improvements in screening and prevention. In 2023, the American Cancer Society estimates that there will be approximately 153,020 new cases diagnosed and 52,550 deaths due to colorectal cancer in the United States.1
Below is a list of the information found within this section:
- Anatomy of the Colon and Rectum
- Risk Factors
- Symptoms
- Detection and Diagnosis
- High Risk Individuals
- Pathology Report & Staging
- Colon and Rectal Cancer Tumor Biology
- Treatment
- Colon and Rectal Cancer Resources
- Section Summary
Anatomy
The colon and rectum are parts of the digestive, or gastrointestinal (GI), system. The purpose of this system is to break down food, absorb nutrients and water, and remove waste from the body.
Food matter is largely broken down in the stomach and then released into the small intestine. Most of the nutrients from food are absorbed in this region of the digestive system. The small intestine continues into the colon, or large intestine, which is divided into 4 regions (based on location): ascending colon, transverse colon, descending colon, and sigmoid colon
The main purpose of the colon is to absorb water and mineral nutrients from the food matter and store waste. Waste moves from the colon into the final 6 inches of the digestive system, called the rectum, and passes out of the body through the anus.
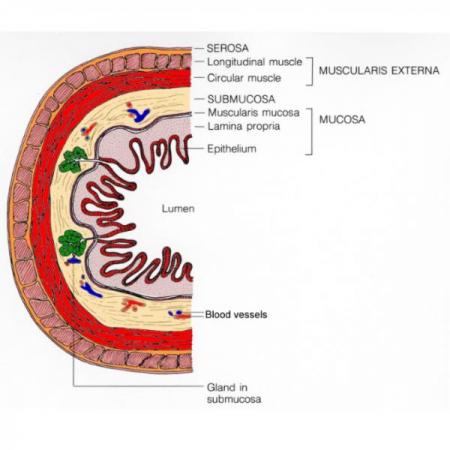
About 95% of colorectal cancers develop in glandular cells that make up the lining of the colon and rectum.2 A cancer that begins in a glandular cell is called an adenocarcinoma. Cancer usually starts in the innermost layer of the lining and slowly progresses through the other layers. The image below is a cross section view of the layers of the colon.
Factors that may influence risk of developing colorectal cancer include3:
- Family History of Colorectal Cancer
- Personal History of Chronic Inflammatory Bowel Disease
- Diabetes
- Age
- Diets rich in red or processed meat
- Excessive drinking of alcohol
- Obesity
- Physical Inactivity
- Smoking
- Makeup of Microbiome
The relative effects of these and other risk factors in any given case of cancer is variable and very difficult to determine with accuracy at this time. Some of these and other risk factors are discussed on the following sections.
Watch a clip about colon cancer prevention and then click here to watch the full interview with Dr. Roberd Bostick.
Family History of Colorectal Cancer
Cancer cases can be grouped into two broad categories, sporadic and familial. Sporadic cancers are those in which the affected individual does not have a known family history of the disease. Familial cancers tend to occur in several generations of a family and affected individuals often have close relatives (brother, sister, father) with the same cancer type. It is possible that these individuals inherit defective genes that lead to the development of a particular cancer type. Individuals with a family history of colorectal cancer are at an increased risk of developing the disease. The degree of risk depends upon the type of relative affected. For example, risk is higher if an immediate family member has been diagnosed with colorectal cancer. The more closely related an individual is to someone with colorectal cancer, the more likely they will share the defective genes. Inherited colorectal cancer accounts for less than 5% of all colorectal cancer cases.4
The two major colorectal cancer susceptibility syndromes are called familial adenomatous polyposis (FAP) and hereditary non-polyposis colorectal cancer (HNPCC):
Familial adenomatous polyposis (FAP): An abnormal growth in the lining of the colon or rectum is called a polyp. Common types of polyps include adenomatous polyps (adenomas), hyperplastic polyps, and inflammatory polyps. Hyperplastic and inflammatory polyps generally do not pose problems. Adenomatous polyps, however, can progress into cancer.5
FAP is a syndrome caused by mutation of the APC (adenomatous polyposis coli) gene. Individuals who are born with this mutation develop hundreds to thousands of adenomatous polyps along their colon and rectum. If left untreated, one or more of these polyps is very likely to progress into cancer.5 The average age of cancer onset in these individulas is 40.6 It is possible to detect and remove adenomatous polyps during screening.
The APC gene will be discussed in the Colorectal Cancer Tumor Biology section of this page and more can be found on the Cancer Genes page.
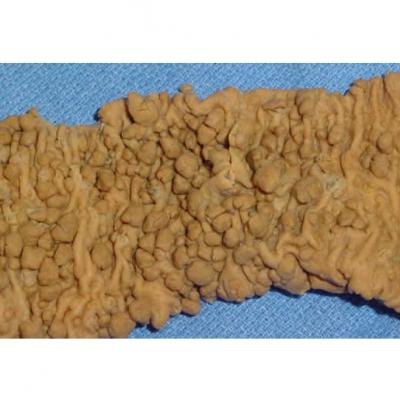
Familial adenomatous polyposis: the mucosal surface of the colon is carpeted with numerous early adenomas. (Image courtesy of: C. Whitaker Sewell, MD - Professor of Pathology, Emory University School of Medicine)
Hereditary non-polyposis colorectal cancer (HNPCC): HNPCC, also called Lynch syndrome, is a syndrome caused by mutation of genes that encode proteins involved in DNA repair, in particular the MLH1, MSH2, MSH6 and PMS2 genes.7 Characteristics of HNPCC include development of cancer by the average age of 45, cancer located in the proximal colon, and increased risk of developing certain cancers located outside the colon.8 HNPCC is not associated with the presence of polyps in the colon or rectum.
The MLH1 and MSH2 mismatch repair genes will be discussed in the Colorectal Cancer Tumor Biology section of this page.
Age
For almost all types of cancer studied to date, it seems as if the transition from a normal, healthy cell to a cancer cell is step-wise progression that requires genetic changes in several different oncogenes and tumor suppressors. This is one reason why cancer is much more prevalent in older individuals. In order to generate a cancer cell, a series of mutations must occur in the same cell. Since the likelihood of any gene becoming mutated is very low, it stands to reason that the chance of several different mutations occuring in the same cell is truly very unlikely. For this reason, the cells in a 70 year old body have had more time to accumulate the changes needed to form cancer cells but those in a child are much less likely to have acquired the required changes. Of course, some children do get cancer but it is much more common in older individuals. More than 90% of patients are diagnosed with colorectal cancer over the age of 50.9 The graph below shows colon cancer rates in the United States as a function of age. The graph was obtained from the National Cancer Institute.10

Dietary Factors
Incidence of colon cancer correlates greatly with certain lifestyle factors, including diet. It is very difficult, however, to identify dietary items that cause a particular cancer. Studies show correlations between chronic heavy alcohol consumption and an increased risk of colorectal cancer.11 On the other hand, some dietary factors are associated with a decreased risk of colorectal cancer. Research suggests that a diet rich in fruits and vegetables may provide a protective effect against the disease.12Calcium is also thought to possibly play a protective role. Studies with labratory animals show that calcium may bind to fatty acids and bile and decrease their harmful effect on the cells that make up the lining of the colon.13 The influence of these dietary factors on colorectal cancer risk is a topic still under debate.
Obesity
Several studies have found an association between increasing body mass index (BMI) and risk of colorectal cancer. The association has been found more consistently in men than in women, however. This difference may be caused by the effect of the female hormone estrogen, which is thought to have a protective effect against colorectal cancer. Women with high body mass indexes tend to have higher estrogen levels compared to women with lower body mass indexes. The higher estrogen levels may counteract the negative effects of an elevated BMI.9
Smoking
Studies have found an association between tobacco use and an increased number of hyperplastic polyps in the colon and rectum. While most do not, hyperplastic polyps may sometimes develop into colorectal cancer. The link between tobacco and hyperplastic polyps appears to be more dependent upon how recently the smoking occurred rather than duration of smoking.14
Prevention of colorectal cancer
There is evidence that taking non-steroidal anti-inflammatory drugs (NSAIDs), such as aspirin, can reduce the development of colon and rectal cancer.15 However, taking NSAIDs is linked to increased bleeding risk; the US Preventive Services Task Force (in 2014) published their recommendations against routine use of NSAIDs for the prevention of colorectal cancer.16 According to the 2013 American Cancer Society Report, consumption of milk and calcium as well as higher blood levels of Vitamin D also appear to decrease colorectal cancer risk.17
Makeup of Microbiome
Studies suggest that bacteria in the gut can be responsible for the growth and spread of tumors. Researchers believe that certain types of gut bacteria help tumors flourish, while others show little to no effect. 18
Symptoms
Symptoms
There are usually no symptoms associated with early-stage colorectal cancer. The American Cancer Society lists the following symptoms associated with more advanced stages of colorectal cancer:19
- Bleeding in the rectum
- Bloody stools (Can be bright red or dark depending on the location of the tumor)
- A change in bowel habits
- Cramps in the colorectal region
- Anemia from the blood loss
- Weakness and fatigue
- Decreased appetite or weight loss
While these symptoms may be caused by factors unrelated to colorectal cancer, it is important to seek medical attention to rule out cancer.
Detection And Diagnosis
The recent development of several colorectal cancer (CRC) screening options has led to the development of complex guidelines and recommendations. There are many different possible combinations of tests yet CRC screening is a cancer prevention tool that is not utilized by many of those who might be helped. Negative perceptions about some of the procedures and the recent application of the test may make them seem unappealing and/or unnecessary.20 CRC is the second-leading cause of cancer death in the United States. CRC screening is both necessary and beneficial. People at high risk for colon cancer should start screening earlier than those with normal risk. After diagnosis there are several options for treatment.
The American Cancer Society's National Guidelines recommend that those 50 and over at normal risk should have regular screening with the following options:20
Detection techniques that identify polyps and cancer:
- Sigmoidoscopy every 5 years, or
- Colonoscopy every 10 years, or
- Double contrast barium enema every 5 years, or
- CT colonography (virtual colonoscopy) every 5 years
Screening Methods that primarily detect cancer20
- Digital rectal examination
- Fecal Occult Blood Tests
- Guaiac Fecal occult blood test (gFOBT) (every year)
- Fecal immunochemical test (FIT) every year
- Stool DNA test (sDNA test) interval uncertain
Colon Cancer Detection: High Risk Individuals
Those at higher risk for colon cancer due to bowel disorders or a family history of the disease should be screened more often and earlier. CRC runs in some families, but there is not always an identified genetic mutation associated with the transmission of the disease. On the other hand, several forms of familial colorectal cancer are associated with specific mutations. These diseases tend to occur at an earlier age. There are several syndromes that fall under this category. For example, familial adenomatous polyposis (FAP) causes the formation of numerous colonic polyps, often numbering in the hundreds. Any of these polyps has the potential to become cancerous. Because of the extreme risk of cancer with this syndrome, patients with a family history of the disease should begin screening at adolesence. Preventative surgery may be performed to prevent cancer formation.
Hereditary Non-Polyposis Colorectal Cancer (HNPCC) is another inherited condition that places individuals at high risk for colon cancer. This syndrome results in the formation of only a few polyps, but they occur at a very young age. It is suggested that people diagnosed with this syndrome be screened every 1-2 years starting at the age of 25 or 10 years prior to the youngest CRC diagnosis in their family. Other syndromes with an increased risk in developing CRC are Peutz-Jeghers syndrome, Juvenile Polyposis, and Cowden syndrome. Testing for these syndromes can have financial and psychological implications. Consultation with a genetic counselor provides patients with their available options.20
Pathology Report And Staging
The Pathology Report
If there is a suspicion that a patient may have colorectal cancer, a sample of of tissue (biopsy) may be taken for examination. After a biopsy is taken, the physician who performed the biopsy sends the specimen to a pathologist. The pathologist examines the specimens at both the macroscopic (visible with the naked eye) and microscopic (requiring magnification) levels and then sends a pathology report to the physician. The report contains information about the tissue's appearance, cellular make up, and whether or not the sample appears to be normal or abnormal. For more information about the pathology report, refer to the Diagnosis & Detection section.
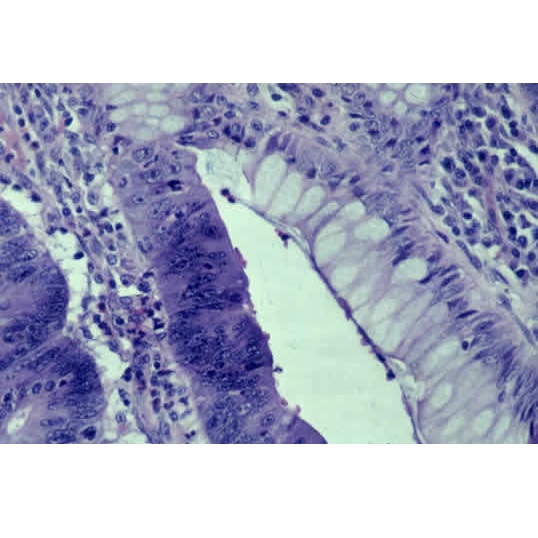
Adenocarcinoma arising within a gland of an adenoma of the colon: Note the very dark staining of the malignant cells, and the presence of nuclei at all levels within the cells. Compare the cells of the adenoma (top of the gland) with the carcinoma cells (bottom portion of the gland)
(Image courtesy of: C. Whitaker Sewell, MD - Professor of Pathology, Emory University School of Medicine)
Staging
Staging a cancer is a way of describing the extent of the disease. One of the most common methods used for colorectal cancer staging is called the T/N/M system, which assigns a degree of severity based on the size, location, and spread of cancer in the body. Other, less widely used methods for colorectal cancer staging are the Dukes system and the Astler-Coller system. Details of the T/N/M system can be found in the Diagnosis & Detection section.
For more details on cancer staging visit the National Comprehensive Cancer Network.
Tumor Biology
Mutation (also known as epigenetic modification) of specific genes alters the behavior of cancer cells. The genetic alterations lead to changes in the amount and/or type of protein product produced by genes (gene expression). As changes accumulate, the cells become more abnormal and cancer progresses. Details about these changes can be found on the Mutation page. Some of the genes that have been shown to be important in the development of colorectal cancer are discussed below:
- APC Gene
- TP53 Gene
- MSH2 and MLH1 Genes
- K-RAS Gene
APC Gene
APC (adenomatous polyposis coli) is a tumor suppressor gene that plays a role in cell signaling. Mutation in APC is thought to be an important step in the initial formation of adenomas.21 Inherited APC mutations result in familial adenomatous polyposis (FAP), a disorder characterized by the growth of hundreds to thousands of polyps along the lining of the colon.
Learn more about APC and cancer development
Learn more about familial adenomatous polyposis (FAP)

Acquired adenomas in the right colon: Two of the larger lesions have developed stalks that connect the neoplastic "head" of the polyp to the mucosal surface. Polyps with stalks are called "pedunculated".
(Image courtesy of: C. Whitaker Sewell, MD - Professor of Pathology, Emory University School of Medicine)
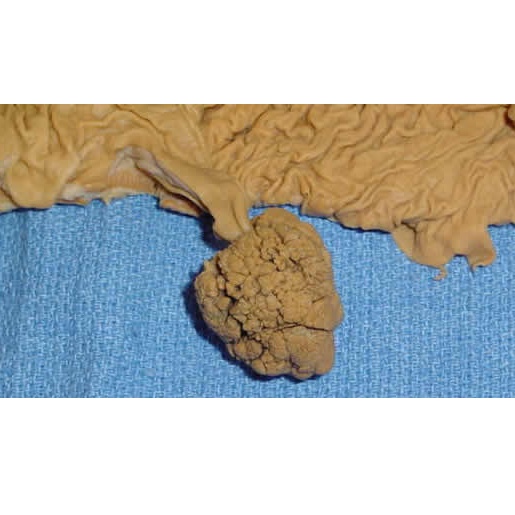
Pedunculated adenoma of the colon: The berry-like "head" of the polyp is the neoplastic portion; the long stalk is composed of normal tissue, and contains the blood supply. (Image courtesy of: C. Whitaker Sewell, MD - Professor of Pathology, Emory University School of Medicine)
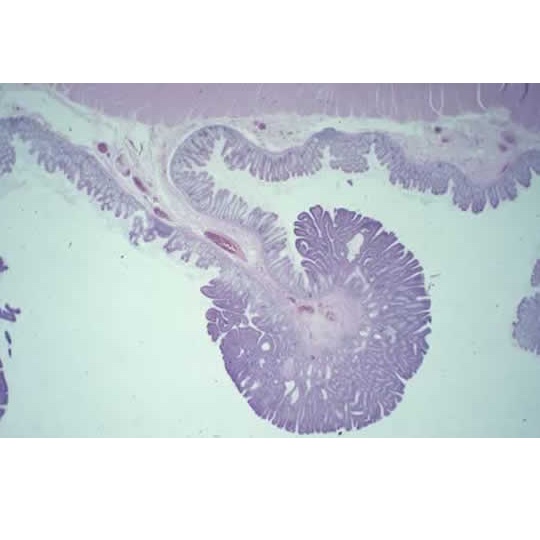
Low power microscopic image of a pedunculated adenoma: The darker staining cells in the head of the polyp represent the mutated neoplastic cells; the stalk is lined by normal colonic mucosa and contains the vascular supply. (Image courtesy of: C. Whitaker Sewell, MD - Professor of Pathology, Emory University School of Medicine)
TP53 Gene
TP53 is a tumor suppressor gene that encodes the protein product p53. TP53 is one of the most common mutations in colorectal cancer and has been associated with resistance to chemotherapy treatment and poorer survival.22
Learn more about abnormal p53 and cancer development
hMSH2 and hMLH1 Genes
About 15% of colorectal cancers develop as a result of non-functional mismatch repair (MMR) genes, in particular the hMSH2 and hMLH1 genes. 7When functional, these genes check over DNA to make sure that all base pairs are matched correctly. Changes in MMR gene expression result from DNA mutation as well as epigenetic changes that alter the activity of genes without changing the actual DNA sequence. Loss of MMR function increases the susceptibility of particular DNA sequences to mutation, a condition known as microsatellite instability or MSI23
K-RAS Gene
K-RAS is a member of a group of genes known as the RAS gene family. These genes encode proteins that play important roles in cell signaling and division. K-RAS is one of the most frequently mutated oncogenes in colorectal cancer.24
Treatment
The treatment of colorectal cancer can be broken down into two categories: early stage and advanced stage. Early stage treatment involves tumors that are confined to the colon or rectum. Advanced stage treatment involves tumors that have spread to other regions of the body. Treatment options are dependent upon size of tumor, location, physical condition of patient, and stage of cancer.
As our focus is on the biology of the cancers and their treatments, we do not give detailed treatment guidelines. Instead, we link to organizations in the U.S. that generate the treatment guidelines.
The National Comprehensive Cancer Network (NCCN) includes the following treatments for colon cancer:
The National Comprehensive Cancer Network (NCCN) includes the following treatments for rectal cancer:
For more information about how these and other cancer treatments work, refer to the Cancer Treatments section.
Information about clinical trials:
- General clinical trial information from CancerQuest
- Click here for information about clinical trials from the National Cancer Institute.
Click here for information about clinical trials from Georgia Clinical Trials Online.
Colon Cancer Resources
Risks for Colon Cancer
Risk Factors Colorectal Cancer (CDC)
Detection and Diagnosis of Colon Cancer
Winship Cancer Institute: Colorectal Cancer Diagnosis and Staging Make an Appointment
Colon Cancer Treatments
Colon Cancer Treatment Guidelines (NCCN)
Colon Cancer Survivorship
Susan Cohan Kasdas Colon Cancer Foundation
Long Term Risks for Colon Cancer Survivors
Side Effects of Colon Cancer Surgery
Late and Long-Term Effects of Treatment
International Colon Cancer Resources
Colorectal Cancer Association of Canada
Colorectal Cancer (Cancer Council Australia)
Section Summary
Introduction
- In the U.S., colorectal cancer is the third most common cancer for both men and women.
- About 95% of colorectal cancers develop in the glandular cells of the lining.
Risk Factors
- Inherited genes play a large role in the formation of colorectal cancer.
- The two major colorectal cancer susceptibility syndromes are called familial adenomatous polyposis (FAP) and hereditary non-polyposis colorectal cancer (HNPCC).
- More than 90% of colorectal cancer patients are over the age of 50.
- A person's diet can increase or decrease his risk for colon cancer.
- Obesity and smoking increase the risk for developing colorectal cancer.
Symptoms
- Typically, early-stage colorectal cancers are asymptomatic.
- Later stages can lead to rectal bleeding, blood in the stool, change in bowel movements, and cramping pain in the lower abdomen.
Pathology Report & Staging
- A biopsy of the tissue can be examined for tissue appearance, cellular make up, and abnormalities.
- The T/N/M system is one of the most common methods used for colorectal cancer staging.
- The T/N/M system assigns a degree of severity based on size, location, and spread of the cancer.
Tumor Biology
- Many genetic changes occur in cancer. Details can be found in the Mutation section.
- One of the more common mutations in colorectal cancer occurs in the APC gene which is a tumor suppressor and plays a role in cell signaling.
Treatment
- Early stage treatment involves cancers confined to the colon or rectum.
- Late stage treatment involves tumors that have spread beyond the colon or rectum.
- Treatments can include: surgery, radiation therapy, chemotherapy, and immunotherapy.
- 1 American Cancer Society.Cancer Facts & Figures 2023. Atlanta: American Cancer Society. (2023). Retrieved from https://www.cancer.org/research/cancer-facts-statistics/all-cancer-facts-figures/2023-cancer-facts-figures.html
- 2 What is Colorectal Cancer? American Cancer Society. (Accessed May 2018) [http://www.cancer.org/Cancer/ColonandRectumCancer/DetailedGuide/colorectal-cancer-what-is-colorectal-cancer]
- 3 Cancer Facts and Figures 2017-2019. American Cancer Society. [https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/colorectal-cancer-facts-and-figures/colorectal-cancer-facts-and-figures-2017-2019.pdf]
- 4 Bodmer WF. "Colorectal polyoposis and inherited colorectal cancer syndromes." Annals of Gastroenterology (2018); 31(1):24-34 [PUBMED]
- 5ab Galiatsatos P, Foulkes WD. "Familial adenomatous polyposis." American Journal of Gastroenterology (2006); 101(2):385-98 [PUBMED]
- 6 Plawski A, Nowakowska D, Podralska M, Lipinski D, Steffen J, Slomski R. "The AAPC case, with an early onset of colorectal cancer." Int J Colorectal Dis (2006) May 19; [Epub ahead of print] [PUBMED]
- 7ab Bandipalliam P. "Germline MLH1 and MSH2 and MSH6 variants in Brazilian patients with colorectal cancer and clinical features suggestive of Lynch syndrome." Cancer Medicine (2018); 7(5):2078-2088 [PUBMED]
- 8 Kohlmann, W. and Gruber SB. "Lynch syndrome." Gene Reviews (2018);(11):1673-1679 [PUBMED]
- 9ab Colorectal Cancer Prevention 2018. PubMed Health. [PUBMED]
- 10 Cancer Stat Facts: Colorectal Cancer represented by the National Cancer Institute. [SEER Colon Cancer Data]
- 11 Rossi, M., Jahanzaib, M., Usman, M., Keshavarzian, A., and Bishehsari, F. "Colorectal cancer and alcohol consumption-populations to molecules." Cancers (BaseI) (2018);10(2). [PUBMED]
- 12 Rada-Fernandez, J., Evans, CEL, Jones, P., Greenwood, DC, Hancock, N., and Cade JE. "Common dietary patterns and risk of cancers of the colon and rectum: analysis from the United Kingdom Women's Cohort Study (UKWCS)." International Journal of Cancer (2018) [PUBMED]
- 13 Marley, AR and Nan, H. "Epidemiology of colorectal cancer." International Journal of Molecular Epidemiology and Genetics (2016); 7(3) 105-114. [PUBMED]
- 14 Ji BT, Weissfeld JL, Chow WH, Huang WY, Schoen RE, Hayes RB. "Tobacco smoking and colorectal hyperplastic and adenomatous polyps." Cancer Epidemiol Biomarkers Prev (2006); 15(5):897-901 [PUBMED]
- 15 Kuo, CN, Pan, JJ, Huang YW, Tsai HJ, and Chang WC. "Association between non-steroidal anti-inflammatory drugs and colorectal cancer: a population-based case-control study." Cancer Epidemiological Biomarkers Prevention (2018). [PUMED]
- 16 Routine Aspirin or Nonsteroidal Anti-inflammatory Drugs for the Primary Prevention of Colorectal Cancer: U.S. Preventive Services Task Force Recommendation Statement. Annals of Internal Medicine. 2014 Oct;146(5):361-364. [https://www.uspreventiveservicestaskforce.org/Page/Document/evidence-summary-aspirin/aspirin-nsaids-for-prevention-of-colorectal-cancer-preventive-medication#notes-copyright-and-source-information]
- 17 Jeon, S. and Shin, E. "Exploring vitamin D metabolism and function in cancer." Nature (2018); 50(20). [https://www.nature.com/articles/s12276-018-0038-9]
- 18 Goodman, B. and Gardner, H. "The microbiome and cancer." The Journal of Pathology; 2018. [PUBMED]
- 19 Signs and Symptoms of Colorectal Cancer 2018. American Cancer Society. [https://www.cancer.org/latest-news/signs-and-symptoms-of-colon-cancer.html]
- 20abcd Colorectal Cancer Screening Tests. American Cancer Society. [https://www.cancer.org/cancer/colon-rectal-cancer/detection-diagnosis-staging/screening-tests-used.html]
- 21 Hankey, W., Frankel, W., and Groden, J. "Functions of the APC tumor suppressor protein dependent and independent of canonical Wnt signaling: implications for therapeutic targeting." Cancer Metastasis Review (2018); 37(1):159-172 [PUBMED]
- 22 Li, A., Li, H., Tang, E., Wu, W., Chen, Y., Jiang, H., Lin, M, and Yin, L. "PIK3CA and TP53 mutations predict overall survival of II/III colorectal cancer patients." World Journal of Gastroenterology (2018); 24(5):631-640 [PUBMED]
- 23 Zeinalian, M., Hashemzadeh-Chaleshtori, M., Salehi, R., and Emami, M. "Clinical aspects of microsatellite instability testing in colorectal cancer." Advanced Biomedical Research (2018); 7:28 [PUBMED]
- 24 Porru, M., Pompili, L. Caruso, C., Biroccio, A., and Leonetti, C. "Targeting KRAS in metastatic colorectal cancer: current strategies and emerging opportunities." Journal of Experimental and Clinical Cancer Research (2018); 37:57 [PUBMED]
